Will Receiveing Momey From Family Affect My Medciad
What is the purpose of wellness insurance?
The IOM articulated the purpose of health insurance in the offset of its six reports: "For individuals and families, health insurance enhances access to wellness services and offers financial protection against high expenses that are relatively unlikely to exist incurred as well as those that are more pocket-size only are all the same not affordable to some."one Three points of elaboration help to explain the mechanisms of health insurance, and to highlight both its potential and its limits. Beginning, wellness coverage helps to connect people with care, in many cases by linking them with a network of providers who participate in their health insurance program. This is how managed intendance and preferred provider organizations work. Second, health insurance lowers financial barriers to access. It does this by reducing out-of-pocket costs for medical care, which disproportionately burden low-income people and people with extensive health care needs. Common measures of financial access to intendance (or lack thereof) include both delayed or forgone care or unmet needs due to toll, and medical cost burden, such as out-of-pocket expenses exceeding some threshold and rates of medical debt and medical bankruptcy.
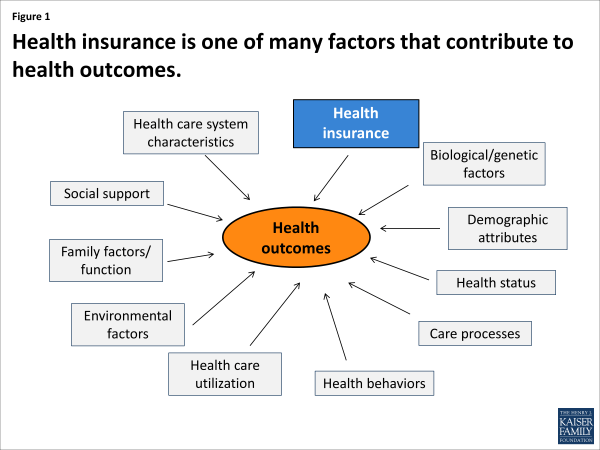
Finally, conceptual models of access and health have identified health insurance as one factor among many, including social, family, genetic, health care system factors and others, whose interaction determines how individuals and populations fare.ii Effigy 1 provides a simplified illustration of just some of the variables at play. Given the circuitous influences involved in determining access, quality, and outcomes, expectations that wellness insurance alone can correct inadequacies in intendance or health disparities, are misplaced. Health insurance cannot overcome systemic barriers to access like health care workforce shortages in low-income communities, or the higher prevalence of chronic diseases in some populations. The impact of health insurance – whether public or individual – needs to be considered in this broader context, and researchers and users of inquiry must inquire whether observed shortfalls in health care outcomes reverberate failures of health insurance or the contribution of other factors that may phone call for different policy responses.
Who are Medicaid beneficiaries?
Medicaid was designed to provide health coverage for low-income children and families who lack access to private health insurance because of their limited finances, health status, and/or severe physical, mental health, intellectual, or developmental disabilities. Medicaid too assists depression-income elderly and disabled Medicare beneficiaries with their Medicare premiums and toll-sharing and covers important benefits that Medicare does non cover, especially long-term intendance. Most states take expanded coverage for low-income children across federal minimum requirements and then that children with family unit income upwardly to at least 200% of the federal poverty level (FPL) are eligible for Medicaid or the Children's Wellness Insurance Program (Flake). [In 2013, 200%FPL was $47,100 for a family of 4] However, state Medicaid eligibility standards for parents are far more restrictive and, in half the states, childless adults under age 65 – no affair how depression their income – are ineligible for Medicaid unless they are disabled or pregnant. Thus, the adult populations studied in most Medicaid research are extremely poor.
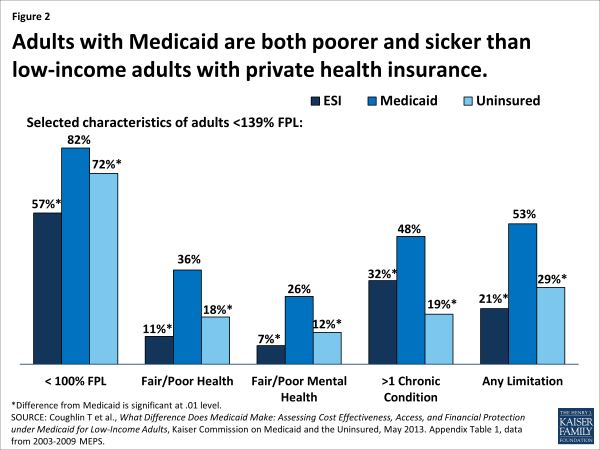
Considering of Medicaid's eligibility criteria and the strong correlation between poverty and poor health and disability, Medicaid beneficiaries are poorer and have a poorer health profile compared with both the privately insured and the uninsured. This is true even within the low-income population, as Figure 2 illustrates for adults. The distinctly higher rates of poverty, chronic illness, and disability in the Medicaid population are important to bear in mind when considering the evidence on Medicaid'due south impact. These disadvantages make access and quality benchmarks that are based on the experience of the privately insured population more challenging to come across in Medicaid. Studies that control for appreciable differences between Medicaid and comparison populations provide a fairer cess of the plan's bear on on access and quality. Even and so, researchers commonly cite as a limitation of their studies the possibility that they did not fully command for underlying population differences that might assistance to explain their findings. This limitation may exist even more than consequential in analyses that examine how health outcomes (equally opposed to access or quality of intendance) compare betwixt Medicaid beneficiaries and other populations, because a larger ready of factors may attenuate the touch of health coverage on outcomes.
Finding #1: Having Medicaid is much better than being uninsured.
Consistently, research indicates that people with Medicaid coverage fare much better than their uninsured counterparts on various measures of access to care, utilization, and unmet need. A large body of evidence shows that, compared to low-income uninsured children, children enrolled in Medicaid are significantly more likely to have a usual source of care (USOC) and to receive well-child care, and significantly less likely to have unmet or delayed needs for medical care, dental care, and prescription drugs due to costs.iii 4 5 6
The inquiry findings on adults generally mirror the patterns for children. A synthesis of the literature on the impact of Medicaid expansions for pregnant women concluded, "…the weight of testify is that expansions led to modest improvements in prenatal care use, in terms of either earlier prenatal care or more adequate prenatal care, at least in some states and for some groups affected by the expansions."7 Mothers covered by Medicaid are much more probable than low-income uninsured mothers to have a USOC, a doctor visit, and a dental visit, and to receive cancer screening services.8 Nonelderly adults covered past Medicaid are more likely than uninsured adults to report wellness care visits overall and visits for specific types of services; they are also more than likely to report timely care and less likely to delay or go without needed medical care because of costs.9 Projections from a recent assay show that, if Medicaid beneficiaries were instead uninsured, they would be significantly less likely to take a USOC and much more than likely to have unmet health care needs; except for emergency department care, their use of key types of services would likewise drop significantly. At the aforementioned fourth dimension, their out-of-pocket spending would increase dramatically – nearly four-fold on average.10 Other research provides evidence of increased access to care and health care utilization for previously uninsured low-income adults who proceeds Medicaid coverage under country expansions of eligibility.11
Recently, the Oregon Health Insurance Experiment has provided uniquely powerful testify about the bear on of Medicaid coverage on uninsured adults.12 13 14 The evidence is compelling because the study is a randomized controlled trial (RCT), the aureate standard in research blueprint. Taking advantage of a lottery held in Oregon in 2008 to allocate a limited number of new Medicaid "slots" for low-income, uninsured nonelderly adults, a team of researchers gathered data on admission, utilization, and clinical health measures for both the adults who gained Medicaid through the lottery and the adults who did not. Two rounds of findings have been published in the New England Journal of Medicine, which tin be summarized, in part, as follows:
- Medicaid increased access to care and health care utilise, and improved self-reported health. One year out from the lottery, the adults who gained Medicaid were 70% more than likely to have a regular place of care and 55% more likely to take a regular md than the adults who did non gain coverage. Associated with more than consequent chief intendance, Medicaid also increased the use of preventive care such every bit mammograms (by 60%) and cholesterol checks (by xx%), and the Medicaid adults had more outpatient visits and hospital admissions and used more than prescription drugs. Finally, the researchers plant that being covered by Medicaid increased cocky-reported health. Compared with the uninsured adults, the Medicaid adults were 25% more likely to report they were in good to fantabulous health (versus fair to poor wellness), twoscore% less likely to report health declines in the concluding six months, and x% more likely to screen negative for depression. The findings 2 years out from the lottery confirmed that Medicaid coverage continued to exist associated with increased access to intendance and health care use, and improved cocky-reported health.
- Medicaid improved adults' mental health markedly; Medicaid'south touch on physical health remains inconclusive. Objective clinical information collected on both groups of adults two years after the lottery testify that, relative to being uninsured, having Medicaid led to a 30% reduction in the charge per unit of positive screens for depression. Gains in physical health were more limited: while Medicaid did increase the detection of diabetes and use of diabetes medication, it did not have a statistically significant effect on diabetes command, or on control of loftier blood pressure or high cholesterol. The researchers note that their study lacked sufficient statistical ability to discover changes, and many of their point estimates are, in fact, inside the range of clinically meaningful changes that would be expected if Medicaid were effective. The authors also identify multiple factors that may mitigate the impact of coverage on clinical outcomes, including unmeasured barriers to access, missed diagnoses, inappropriate medication, patient noncompliance, and ineffectiveness of treatments.
- Medicaid virtually eliminated catastrophic medical expenses. Catastrophic out-of-pocket spending (divers as costs exceeding thirty% of income) was most eliminated among the adults who gained Medicaid coverage. Likewise, the likelihood of having medical debt was reduced by more than 20%, and having Medicaid had a meaning impact on all cocky-reported measures of financial strain due to health care costs, including borrowing money or skipping other bills to pay medical bills and existence refused treatment due to medical bills in the past six months.
Analyses that examine how Medicaid beneficiaries with serious chronic illnesses, such equally diabetes, fare are of detail involvement considering of the prevalence of these conditions in the Medicaid population and the consequences if care is lacking. A recent series of studies focused specifically on low-income nonelderly adults with major chronic diseases shows statistically pregnant and clinically important differences between Medicaid beneficiaries and the uninsured on of import measures of access and care. For case, adults with diabetes who are covered by Medicaid are less likely than those who lack insurance to report delaying or being unable to get needed care. They also accept more function visits, fill more prescriptions, and are more likely to receive the key elements of recommended diabetes intendance.15 The two related studies on other major chronic illnesses show like results.16
Continuity in Medicaid coverage makes a difference. Research has shown that interruptions in Medicaid coverage tin can pb to greater emergency section utilize besides as significant increases in hospitalization for weather condition that tin be managed on an ambulatory basis.17 18 19 Studies examining the short-term impacts of loss of Medicaid coverage provide additional show of Medicaid'south affect. Studies in California and Oregon of low-income adults who lost their Medicaid coverage establish significant declines in bones measures of access, such as having a USOC, unmet health care and medication needs, and likelihood of a contempo primary care visit, equally well as meaning declines in health status.20 21 In focus groups conducted with adult Medicaid beneficiaries in Massachusetts following the state'south elimination of adult dental benefits, nearly all the participants reported serious oral wellness problems that, for many, resulted in chronic and serious pain.22
Beyond showing improved admission to care and utilise of recommended treat Medicaid beneficiaries relative to the uninsured, research as well provides evidence that broader eligibility for Medicaid at the state level is associated with significant reductions in both child mortality23 and adult mortality.24 A study examining the relationship between broader state Medicaid coverage of adults and admission to physician and preventive services plant that college levels of Medicaid coverage were associated with essentially improved access to care for all low-income adults in the state, and as well that access gaps between depression- and high-income adults were substantially larger in states with limited Medicaid coverage than in states with broader coverage.25
Finding #2: Medicaid beneficiaries and the privately insured have comparable access to preventive and chief care.
Given the benefits that cascade as wellness insurance lowers financial barriers and opens the door to the wellness care system, and, in contrast, the downstream deficits in care that the uninsured experience, measures of access to preventive and primary care, like having a USOC, receipt of a well-kid visit, and cancer screening rates, tin be seen non just as process measures or ends for their own sake, but as the anchors of loftier-quality care. Appropriately, how Medicaid beneficiaries do on these bones access measures is an important indicator of the quality of intendance in Medicaid. Many studies have used the experience of privately insured individuals as a benchmark for gauging Medicaid'due south performance.
Children with Medicaid and privately insured children compare quite closely in their access to and use of preventive and primary care. Nationally, more than 95% of both groups of children accept a USOC, and the very small percentage who report delaying or going without needed care due to cost in the past year is the same betwixt the two groups, which is notable because the lower income and greater wellness intendance needs of children covered by Medicaid.26 The most recent almanac HHS report on the quality of care for children in Medicaid and CHIP concluded that children are similarly likely to have had a main care visit in the past twelvemonth whether they are publicly or privately insured.27 Younger children with public coverage appear to lag behind privately insured children on well-child visit rates and immunization rates, but adolescents with Medicaid or Flake may fare also as or better than adolescents with individual coverage.
A recent report prepared for the Medicaid and Scrap Payment and Admission Commission (MACPAC) reached similar findings when comparisons between publicly and privately insured children were adjusted for health, demographic, and socioeconomic differences between the 2 groups.28 It also found that children with public coverage are every bit likely equally privately insured children to take had a specialist visit in the past year. At the same fourth dimension, the report identified of import measures of access on which Medicaid children fare slightly worse than those with individual insurance. For case, they are less likely to have a USOC with night or weekend hours and are more than likely to delay care for this reason. They are too more probable to lack transportation to the doctor'south office or dispensary.
A companion study for MACPAC on adults enrolled Medicaid found that, when health, demographic, and socioeconomic differences were controlled for, Medicaid adults did also as or meliorate than privately insured adults on key measures, including USOC and receipt in the past year of a routine check-upwardly, a general dr. visit, a specialist visit, a mammogram, and flu vaccination.29 The shares of Medicaid and privately insured adults reporting any unmet needs due to costs were comparable, but Medicaid adults were significantly less likely to report unmet needs for medical care, prescription drugs, and mental health care, compared with privately insured adults. These results are largely consistent with findings from other studies comparison Medicaid and privately insured adults' admission and utilization.30 31 32 A review of the literature on Medicaid's bear upon on birth outcomes concluded that, when known take a chance factors for preterm nascence and low birth weight are controlled for, birth outcomes are not different betwixt women with Medicaid and privately insured women.33 Medicaid also provides greater financial protection than private health insurance.34,35 Research estimating how Medicaid beneficiaries would fare if they had private insurance instead projects that their out-of-pocket spending would increment more than three-fold on average, and that out-of-pocket burden would exist heaviest for the subgroup of individuals with health limitations.36
Finding #3: Specialists are less willing to take Medicaid patients than privately insured patients. However, studies comparing access to specialist care between Medicaid and private insurance have produced mixed findings – likely a reflection of the difficulty of adjusting for all the factors that may influence access.
Equally distinct from access to primary care, access to specialty care has emerged in some research as a weakness in Medicaid relative to private insurance. A review of the literature on children's access to specialty care constitute that Medicaid children announced less likely than privately insured children to receive specialist intendance for various atmospheric condition and more likely to have trouble finding a physician willing to accept their insurance.37 Data included in the HHS study on Medicaid and Chip children mentioned before bear witness that fewer than one-half of parents with children enrolled in Medicaid or CHIP said it was always easy to get an appointment with a specialist, and the written report cites admission to specialty intendance as an area of item concern. Consequent with those results, "secret shopper" and other studies have found specialist physicians and clinics far more likely to deny appointments to Medicaid and CHIP children than to privately insured children, and much longer wait times for appointments for publicly insured children.38 39 At the aforementioned time, the report for MACPAC, also mentioned earlier, found that observed gaps in access to specialty between publicly and privately insured children disappeared when demographic besides as health status differences between the two groups were controlled for.
In a nine-city inspect study investigating adults' access to specialist care, 64% of callers saying they were privately insured, but but 34% of those maxim they had Medicaid, were able to secure an engagement for urgent follow-up intendance for iii serious atmospheric condition, suggesting that Medicaid adults may lack adequate access to specialist intendance.40 However, the report for MACPAC on adults cited earlier determined that privately insured adults are no more than or less probable than Medicaid adults to have a specialist visit. Information technology showed that, when health status and demographic differences between the two groups are controlled for, the two groups are equally likely to accept specialist visits overall, specialist visits excluding OB/GYN visits, and, for women, OB/GYN visits.41 This finding is at variance with the finding from another assay, which projected that, if Medicaid adults were instead covered by individual insurance, their apply of specialists would exist significantly college.42
Finding #four: Studies examining the causes of higher emergency department (ED) employ by Medicaid beneficiaries compared to the privately insured betoken that most of the departure is due to college rates of symptoms adamant by ED triage staff to need urgent attending. Barriers to access to care are also a factor.
Compared with both privately insured people and the uninsured, Medicaid beneficiaries have much higher rates of ED use.43 Nevertheless, a substantial body of enquiry investigating this disparity more than closely indicates that poorer health and access challenges in Medicaid both play important roles in explaining Medicaid's higher ED visit rates.
A study issued about a twelvemonth ago showed that only a small-scale portion of Medicaid patients' higher ED use was explained by visits for non-urgent symptoms. Most of the Medicaid-private deviation was attributable to more ED visits by Medicaid patients for symptoms that were judged by ED triage staff to need urgent or semi-urgent evaluation. Compared to nonelderly privately insured people, nonelderly Medicaid patients had near double the rate of ED visits both for symptoms needing evaluation inside an hour and for those needing evaluation within 1 to 2 hours.44 Also, compared with the privately insured adults with ED visits, the Medicaid adults were more likely to accept a secondary diagnosis of a mental disorder, and their visits were more than probable to involve more than one major chronic condition and more probable to involve a disability.
Other enquiry provides evidence that increased ED utilization is associated with barriers to timely primary care, and that more than accessible afterwards-hours intendance is associated with lower rates of ED visits.45 46 A study examining the reasons for ED visits past nonelderly adults points in this direction; the results prove that, compared with the privately insured with ED visits, Medicaid adults with ED visits were much more likely to study that they had no other place to get and that their doc's office or clinic was not open.47 A written report probing factors associated with specialists' willingness to take children with public health insurance identified referral through infirmary EDs as a common mechanism past which primary care physicians secure this care for their Medicaid and CHIP patients.48 The results from a recently published qualitative study seeking to identify the reasons that people of low socioeconomic status prefer hospital care to convalescent care indicate that patients, too, see increased access to specialty care every bit one important reward of seeking care in a hospital setting. Medicaid patients reported that while the direct costs of an ED visit and a physician office visit were like, the overall cost associated with an office visit was greater considering of the boosted time and expense required for specialty visits or tests recommended by the primary care provider. Transportation likewise emerged as an effect. Finally, many patients reported that when they called physicians' offices, they were advised to go to the ED.49
Finding #v: New evidence is emerging almost the quality of care provided to Medicaid beneficiaries.
Research investigating the quality of care received by Medicaid beneficiaries is limited, just two new analyses, one focused on health heart care and the other on infirmary care, indicate that the care received by people with Medicaid coverage tracks closely with benchmarks for high quality.
Health eye care
Health centers are a key source of preventive and primary intendance for medically underserved communities and populations, including millions of Medicaid beneficiaries. The ACA funded a major expansion of the health centre program to help run into the expected increased demand for care as both Medicaid and private coverage expand. Given the role of health centers in providing intendance to Medicaid patients, evidence on the quality of care they deliver is important to an assessment of the Medicaid program itself. A recent study examined how wellness center operation on a set of three quality measures – diabetes control, claret pressure command, and receipt of a Pap test within the past three years – compares to the performance of Medicaid managed intendance organizations (MCOs), which likewise serve a low-income population.50 The study divers the standard for "high operation" as the 75thursday percentile of Medicaid MCO quality scores, and the standard for "lower operation" as the mean Medicaid MCO quality score. Because all Medicaid MCO enrollees are insured but a large share of health eye patients are uninsured, MCO performance is a demanding benchmark to employ for wellness centers.
The report produced the following key findings:
- More than ane in 10 health centers have consistently high functioning relative to Medicaid MCOs. Of 1,200 health centers total, 130 outperformed iii-quarters of Medicaid MCOs on all three measures of chronic and preventive care. Moreover, the average quality scores for these wellness centers exceeded the MCO high-operation benchmark by at least 10 percentage points on each measure out. Many boosted wellness centers were high-performing on individual measures, although not on all three – 80% met or exceeded the MCO high-performance standard for diabetes control, and over half did so for blood pressure control. Fewer than 4% of health centers were lower-performing on all 3 measures. However, in 70% of all health centers, Pap examination rates trailed the average Medicaid MCO score, highlighting an of import gap in the quality of preventive treat women.
- The consistently loftier-performing health centers were concentrated in certain states, as were consistently lower-performing health centers. A bulk of states had at least ane consistently high-performing health center, just one-tertiary of such high-performers were in California, New York, and Massachusetts, where just xviii% of all health centers are located. Similarly, ane-third of the consistently lower-performing health centers were concentrated in three states – Louisiana, Texas, and Florida – that business relationship for simply over 10% of all health centers.
- Health centers with consistently lower performance are distinguished past extremely high uninsured and homeless rates. In the wellness centers that lagged behind average Medicaid MCO functioning on all 3 quality measures, fully half the patients were uninsured, and well over one-tertiary were homeless. The lower functioning of these health centers probably says more near the profile of their patients and the limited resources available to health centers with high proportions of uninsured patients with complex health needs than most the quality of care provided to them. The higher rates of both private and Medicare coverage observed in the consistently high-performing health centers suggest that broader coverage equally the ACA is implemented could help conductor improvements in wellness center quality.
Infirmary care
A team of Harvard researchers conducted a study to compare the quality of infirmary care received past nonelderly adults covered by Medicaid and by private insurance, respectively, for 3 major atmospheric condition: heart attack, congestive center failure, and pneumonia.51 Considering the recommended processes of care for all these conditions are supported past strong scientific evidence, the researchers used "perfect intendance" – the receipt by an individual of all indicated processes of intendance – to gauge the quality of hospital care. Perfect-intendance scores for Medicaid patients and private-pay patients were calculated by accumulation the individual-level information by payer, both nationally and for each state.
The study found that:
- Medicaid and privately insured patients receive hospital care of very similar quality . The written report constitute statistically significant just modest differences at the national level between the shares of Medicaid and privately insured adults who received perfect care. Perfect-care scores were higher for privately insured patients, only the differences were between 1% and three%. Land-level differences in hospital quality between Medicaid and private-pay patients were besides small – less than 3 percentage points on average. The largest Medicaid-individual difference in a state was xiv percent points for heart attack care, only fewer than x states had differences larger than 5 per centum points for whatever of the 3 conditions.
- State variation in the quality of hospital care Medicaid patients receive likely reflects geographic variation in how hospital care is delivered rather than land Medicaid policies. Notably, the researchers found significant variation in the quality of hospital intendance from state to country. Even so, quality tended to be higher for Medicaid patients where information technology was also higher for the privately insured, and lower for Medicaid patients where it was lower for the privately insured. The strong correlation in quality between Medicaid and privately insured patients suggests that the factors driving the quality of hospital intendance for Medicaid patients have more to do with how hospital care is delivered geographically, by state, than with factors related to state Medicaid policies.
Conclusion
In its totality, the research on Medicaid shows that the Medicaid plan, while not perfect, is highly effective. A large body of studies over several decades provides consequent, stiff prove that Medicaid coverage lowers financial barriers to access for depression-income uninsured people and increases their likelihood of having a usual source of care, translating into increased utilize of preventive, master, and other care, and improvement in some measures of health. Furthermore, despite the poorer health and the socioeconomic disadvantages of the low-income population it serves, Medicaid has been shown to meet demanding benchmarks on important measures of access, utilization, and quality of care. This evidence provides a solid empirical foundation for the ACA expansion of Medicaid eligibility to millions of currently uninsured adults, and individuals and communities affected by the Medicaid expansion can be expected to benefit significantly. At the same time, the Medicaid program cannot overcome health care organization-wide problems, similar gaps in the supply and distribution of the health care workforce, or lack of access to transportation in depression-income communities. Nor tin Medicaid exist expected to tackle many other barriers and issues that disproportionately affect depression-income individuals and communities. These challenges require an additional set of policy responses beyond Medicaid'due south ambit.
Nevertheless, Medicaid can be further strengthened by addressing recognized shortcomings in the electric current program. Securing acceptable provider participation in Medicaid remains a key challenge. Improving continuity in Medicaid coverage is necessary to ensure that beneficiaries are able to obtain timely care and uninterrupted management of their chronic illnesses and disabilities. Rigorous oversight of the chance-based managed care arrangements in which more and more Medicaid beneficiaries receive their care is needed, especially equally states expand managed care to people with more complex needs. New models of more coordinated and integrated care, and payment approaches that support them, are also needed. States are moving forward on all these fronts, often leading the way, and increased resources and flexibilities provided by the ACA proceed to accelerate their progress. With stable and adequate federal and state investment in Medicaid, and state actions that leverage the purchasing ability of the plan to drive higher quality, Medicaid'southward demonstrated potential to amend access and care for depression-income people can be optimized.
Source: https://www.kff.org/report-section/what-is-medicaids-impact-on-access-to-care-health-outcomes-and-quality-of-care-setting-the-record-straight-on-the-evidence-issue-brief/
Post a Comment for "Will Receiveing Momey From Family Affect My Medciad"